Tetralogy of Fallot (TOF) Treatment
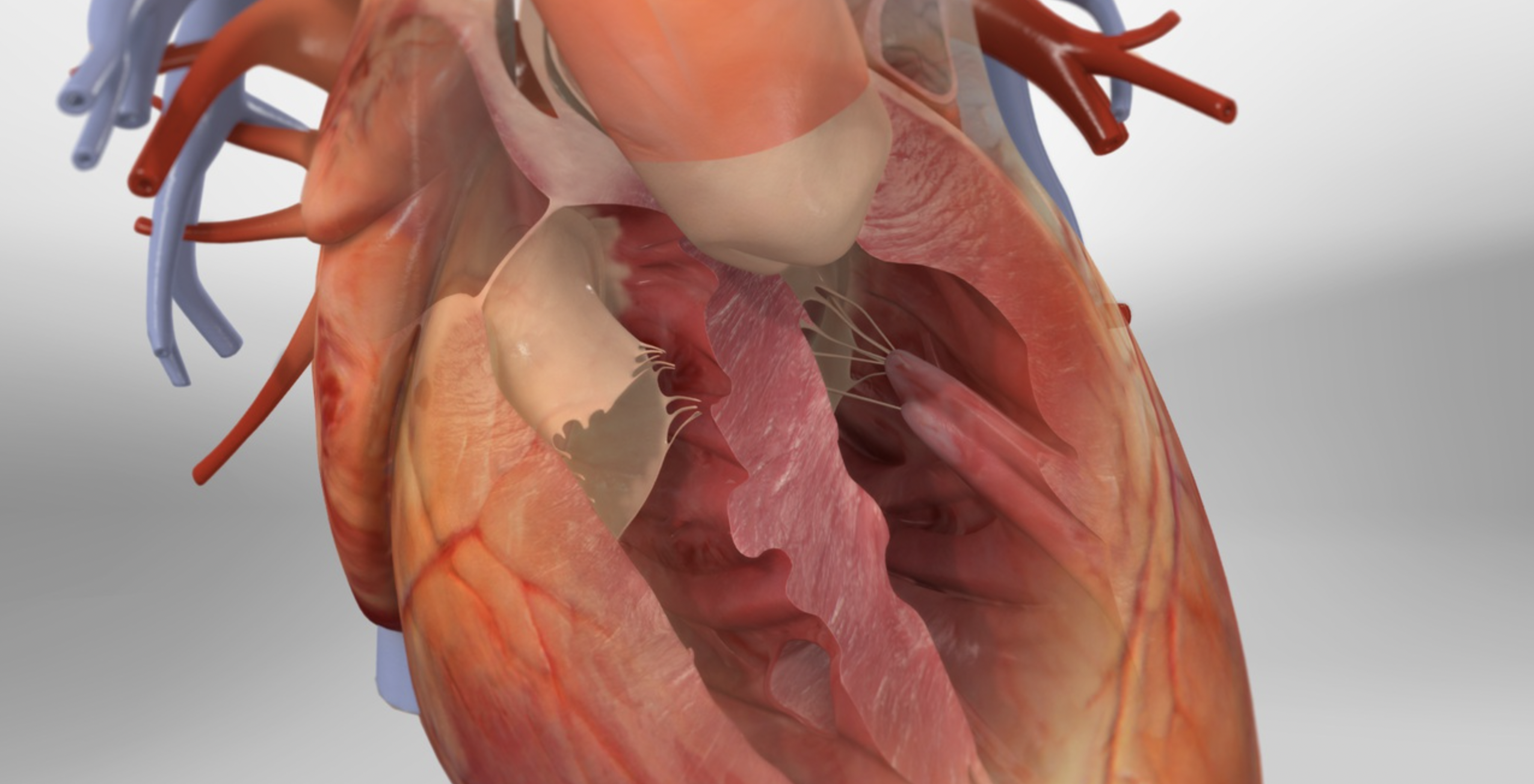
Tetralogy of Fallot (TOF) is a rare and complex congenital (at birth) heart defect that affects the structure and function of the heart. This condition is composed of four anatomical abnormalities resulting in oxygen-poor blood being pumped out of the heart and into the rest of the body. These defects occur together as a unit and include:
- Ventricular Septal Defect (VSD): A hole between the heart’s lower chambers.
- Pulmonary Stenosis: Narrowing of the pathway from the right ventricle to the lungs.
- Right Ventricular Hypertrophy: Thickening of the right ventricle’s muscular wall.
- Overriding Aorta: The aorta is positioned above both ventricles, receiving blood from both, leading to a mix of oxygenated and deoxygenated blood being circulate
The primary treatment for TOF in Cuba is intracardiac repair, ideally performed within the first year of life. This procedure involves closing the ventricular septal defect (VSD) with a patch and widening the narrowed pulmonary valve and arteries to improve blood flow to the lungs. For some patients, a temporary surgery, Blalock-Taussig shunt, may first be performed to increase blood flow to the lungs before the complete repair.
If TOF is left untreated, it can lead to significant consequences with a significant reduction in quality of life. The most prominent complications include:
- Chronic low oxygen levels in the blood.
- Cyanosis.
- Poor growth and development in children.
- Frequent episodes of fainting or seizures due to lack of oxygen.
- Increased risk of infections such as endocarditis.
- Heart failure.
- Shortened lifespan.
Types of Tetralogy of Fallot
TOF variation is based on the severity and specifics of the heart defects involved. While the classic form of TOF includes the four key defects, their exact nature, the degree and combination of these defects can vary. These variations may have an impact on the severity, clinical presentation, and course of treatment for people with TOF. Some of the variations include:
- TOF with Pulmonary Atresia: In this type, the pulmonary valve is completely closed with no direct blood flow from the right ventricle to the lungs.
- TOF with Absent Pulmonary Valve Syndrome: In this variation there is an absence of or severe malformation of the pulmonary valve, leading to significant airway compression and respiratory issues.
- TOF with Atrioventricular Septal Defect: This form is a combination of TOF defect with another defect (atrioventricular septal defect – AVSD), where there is a large hole in the center of the heart affecting both the atria and ventricles.
Causes
The precise cause of TOF is not always clear, however, a combination of genetic and environmental factors during fetal development are believed to be factors contributing to the development condition.
- Genetic Factors: Genetic mutations, chromosomal disorders and other genetic syndromes can affect the normal formation of the heart during fetal development.
- Environmental Factors: Maternal health, maternal infections (such as rubella), medications and substance use during pregnancy or poor maternal nutrition, particularly a lack of folic acid, has been associated with an increased risk of congenital heart defects.
- Unknown Factors: In a large number of cases, the exact cause of TOF cannot be identified.
Symptoms
Symptoms of TOF can vary depending on the severity of the condition and may include:
- Cyanosis: A bluish tint to the skin, lips, and nails due to low oxygen levels in the blood.
- Difficulty Breathing: Especially noticeable during feeding or physical activity.
- Heart Murmur: An abnormal heart sound.
- Clubbing: Enlargement of the fingers and toes.
- Poor Weight Gain: Infants may struggle with feeding and growth.
Diagnosis
Tetralogy of Fallot (TOF) is typically diagnosed with a combination of steps, including a combination of clinical evaluation, imaging studies, and other diagnostic tests.
- Clinical Evaluation: Medical History including family history and physical examination.
- Echocardiogram: This is a non-invasive test that uses ultrasound waves to produce detailed images of the heart’s chambers and valves, revealing their structure and function. It can accurately show the four characteristic defects.
- Chest X-ray: A chest X-ray can reveal the size and shape of the heart and lungs. In TOF, the heart may appear boot-shaped due to right ventricular hypertrophy. Additionally, it helps identify any associated lung abnormalities or complications, such as increased pulmonary blood flow or lung congestion.
- Electrocardiogram (ECG or EKG): An ECG records the electrical activity of the heart and can help identify abnormal heart rhythms and right ventricular hypertrophy, both common in TOF. By identifying these electrical patterns, the ECG helps confirm the presence of TOF and assesses the severity of the heart’s structural abnormalities
- Pulse Oximetry: This is a non-invasive measurement of oxygen saturation levels in the blood and can quickly and accurately detect hypoxemia
- Cardiac Catheterization: In some cases, a cardiac catheterization may be performed. A thin, flexible tube (catheter) is inserted into a blood vessel and guided to the heart. This procedure provides detailed information about the heart’s structure and blood flow and can measure pressures within the heart chambers and blood vessels.
- Magnetic Resonance Imaging (MRI) or CT scan: These images provide highly detailed depiction of the heart and surrounding structures, including the size and position of the ventricular septal defect (VSD), the extent of pulmonary stenosis, the degree of right ventricular hypertrophy, and the location of the overriding aorta. MRI and CT scans can also identify associated anomalies and complications, such as abnormalities in the pulmonary arteries or aortic arch.
- Blood Tests: Blood tests are an important in the diagnosis and management of TOF since they provide information on the overall health of the patient, can detect infections, monitor electrolyte levels and metabolic function and measure hemoglobin and hematocrit levels to assess oxygen-carrying capacity.
Treatment options:
Treatment approach for TOF can vary depending on the severity of the condition and the patient’s overall health; however, the primary approach involves surgical intervention, usually performed in early infancy.
Initial Medical Management
For some patients initial medical management to stabilize their condition may be required. This may include prostaglandin infusions, Beta-Blockers and oxygen therapy.
Surgical Intervention
Surgical intervention is carried out to correct the anatomical defects and improve the blood flow to the lungs and the rest of the body.
- Intracardiac repair: This is the most common surgical procedure for TOF and is usually performed between three to six months of age. The procedure involves:
- Ventricular Septal Defect (VSD) Closure: The surgeon places a patch over the VSD to close the hole between the right and left ventricles, preventing the mixing of oxygen-poor and oxygen-rich blood.
- Relief of Pulmonary Stenosis: The narrowed pulmonary valve and the infundibulum (the area just below the valve) are widened to improve blood flow to the lungs.
- Right Ventricular Outflow Tract Reconstruction: The right ventricular outflow tract (RVOT) may be widened using a patch, ensuring unobstructed blood flow from the right ventricle to the pulmonary artery.
Temporary Procedures
Some patients, especially infant who are too small or not stable enough for a complete repair, temporary procedures may be performed:
- Blalock-Taussig Shunt: A shunt is placed between the subclavian artery and the pulmonary artery to increase blood flow to the lungs to improve oxygenation until the baby is ready for intracardiac repair.
- Balloon Pulmonary Valvuloplasty: This is a minimally invasive procedure that involves inflating a balloon to widen the pulmonary valve to improve blood flow to the lungs.
Postoperative Care
After surgery, patients require meticulous postoperative care and long-term follow-up to monitor their heart function and overall health, for pain management and infection prevention.
In some cases, patients may require further interventions or surgeries later in life:
- Pulmonary Valve Replacement: Over time, the repaired pulmonary valve may become leaky or stenotic again, necessitating a valve replacement.
- Right Ventricular Outflow Tract (RVOT) Revision: If the RVOT becomes narrowed or obstructed, additional surgery may be needed to correct the issue.
ACCOMMODATION
Private room with the following features:
- Electronic patient bed
- Equipment for disabled patient
- Oxygen hookup
- Three AP meals taking into account the patient’s preferences and / or special diets prescribed by physician
- Fully equipped private bathroom
- Infirmary and nursing care
- Colour TV with national and international channels
- Local and international phone services (extra cost will apply)
- Safe box
- Internet service on every floor
- Laundry services
- Assistance in visa issuance and extension (If needs be)
- Each patient/ companion will be assigned a multi-lingual field member with the mandate of attending to all of our patients’ translation and personal needs;
- 20 hours internet service;
- Local airport pickup and drop off; and
- Hospital pickup and drop off (if needed)
